EYE TRAUMA 2026: ASOT ANNUAL MEETING & SKILLS TRANSFER LAB
April 24-26, 2026 | Houston Methodist Institute for Technology, Innovation and Education (MITIE) | Houston, TX
2026 Comprehensive Skills Transfer Wet Lab
The ASOT Wet Lab is a tiered, skills-based surgical curriculum designed to train ophthalmologists across all levels — from medical students to subspecialty surgeons — in the management of ocular trauma. The program integrates anterior and posterior segment techniques, orbital trauma, diagnostic technology, and advanced reconstruction in a structured, progressive format. The lab benefits from hosting global faculty representing subspecialty expertise from across the world.
Damage Control Ophthalmology
7:30am-12:35pm (Limit 54)
Audience: PGY-2 through Attending Level
This core curriculum focuses on the first critical steps in ocular trauma stabilization and repair. This includes orbital and adnexal injury, and open and closed globe trauma. Designed for residents, fellows, and practicing ophthalmologists, this component emphasizes surgical decision-making, tissue preservation, and complication management in open and closed globe injury.
Appropriate For
- PGY-2 to PGY-4 residents
- Ophthalmology fellows
- Comprehensive ophthalmologists
- Subspecialty ophthalmologists
- Trauma-call faculty
Lab Components
Zone 1: Corneoscleral Open Globe Repair
This station builds competence in primary globe closure and anterior segment stabilization.
Skills Developed
- Repair of simple and complex corneal lacerations
- Slip-knot technique for corneal closure
- Management of iris and vitreous prolapse
- Lensectomy in traumatic cataract
- Anterior chamber washout
- Management of anterior chamber IOFB
- Fish hook removal from corneal stroma
Clinical Competencies
- History-taking and surgical planning for anterior segment trauma
- Recognition and management of wound leaks
- Decision-making in staged vs definitive repair
Zone 2 & 3: Posterior Corneoscleral Open Globe Repair
This station is ideal for posterior open globe repair, including ruptures and lacerations, while preserving uveal tissue and managing vitreous and uveal prolapse.
Skills Developed
- Scleral and limbal laceration repair
- Peritomy with relaxing incisions
- Extraocular muscle isolation and reattachment
- Management of vitreous and uveal prolapse
- Anterior and posterior tap/inject techniques
- Vitreous culture and antimicrobial injection strategies
- Discussion of timing for vitrectomy and IOFB removal
Clinical Competencies
- Surgical planning for posterior extension injuries
- Understanding staged trauma reconstruction
- Management of closed globe posterior injuries
Orbit & Adnexal Trauma
This station emphasizes eyelid and orbital anatomy, layered closure of the skin and eyelid, and emergency orbital intervention.
Skills Developed
- Full-thickness lid margin repair
- Canalicular probing and repair
- Tarsal plate reapproximation
- Lateral canthotomy and cantholysis
- Full-thickness lid decompression
- Enucleation techniques
- Extraocular muscle securing
- Retrobulbar block practice
Clinical Competencies
- Recognition and management of orbital compartment syndrome
- Indications for enucleation
- Timing of orbital fracture repair
- Layered wound closure and anatomic reconstruction
Diagnostic & Surgical Technology Exhibit
This component of the lab bridges cognitive decision-making with modern surgical technology, allowing surgeons to experience diagnostic and surgical tools that they may want to incorporate into trauma care.
Skills Developed
- Ophthalmic ultrasound interpretation
- Retinal laser system utilization
- Phacoemulsification and vitrectomy machine setup
- Microscope and heads-up display customization
- IOFB forceps and intraocular magnet use
- EyeSi surgical simulator practice
- Ocular Cohearance Tomagraphy and Corneal Topography
Clinical Competencies
- Equipment selection in trauma cases
- Preoperative and postoperative imaging integration
- Optimization of surgical platforms for trauma repair
Early Career Wet Lab
8:00am – 12:30pm (Limit 32)
Audience: Pre-ophthalmology medical students through early PGY-2
This foundational curriculum introduces microsurgical principles and ocular trauma fundamentals in a highly structured environment. This curriculum will establish the microsurgical foundation required for safe progression to more advanced trauma management.
Appropriate For
- Medical students
- PGY-1 residents
- Early PGY-2 residents seeking fundamentals refresh
Lab Components
Corneal Suturing & Microscope Handling
Skills Developed
- Basic corneal suturing (simple interrupted)
- Instrument handling and ergonomics
- Microscope visualization and depth perception
- Knot tying with appropriate tension
- Error recognition and correction
Clinical Competencies
- Understanding tissue tension
- Recognition of poor suture placement
- Introduction to globe integrity principles
- Ocular Trama Lectures
Basic Skin Suturing
Skills Developed
- Simple interrupted skin closure
- Instrument positioning and hand control
- Layered closure fundamentals
Clinical Competencies
- Understanding soft tissue repair
- Recognition of appropriate tension and spacing
Slit Lamp, Corneal Foreign Body & Seidel Testing
Skills Developed
- Corneal foreign body removal
- Rust ring burr technique
- Seidel testing for wound leak
- Slit-lamp examination fundamentals
Clinical Competencies
- Risk assessment of corneal injury
- Recognition of possible IOFB
- Decision-making regarding globe integrity
Subspecialty Reconstruction
Wet Labs
1:00pm-4:30pm (Limit 10/subspecialty, can only pick one)
Audience: PGY-4, Senior Residents, Fellows, and Attending Surgeons
Designed for surgeons who have completed residency or are in advanced training, this curriculum focuses on complex anterior and posterior segment reconstruction following trauma.
Appropriate For
- Ophthalmologists who are completing residency or are in fellowship or in practice
- Cornea and glaucoma specialists
- Retina fellows and attendings
- Trauma surgeons in tertiary centers
Lab Components
Complex Anterior Segment Lab
Limit 10
Iris and Cyclodialysis Repair / Yamane IOL Scleral Fixation / Artificial Iris Certification
Skills Developed
- Iris repair using prolene sutures
- Intraocular knot tying
- Cyclodialysis repair
- Secondary IOL placement using Yamane scleral fixation
- Corneal BrightMEM Placement
Clinical Competencies
- Managing traumatic aphakia
- Decision-making in lens fixation options
- Reconstruction after anterior segment tissue loss
Iris Prosthesis Implantation (pre-lab training required for certification: click here login: iris1400)
Skills Developed
- Preparation and implantation of iris prosthesis
- Iris prosthesis indications assessment
- Device handling and positioning
Clinical Competencies
- Reconstruction for traumatic aniridia
- Visual rehabilitation considerations
Hyphema Washout / Glaucoma Tube Placement
Limit 10
Hyphema Washout
Skills Developed
- Anterior chamber washout techniques
- Management of traumatic hyphema
- Surgical evacuation strategies
Clinical Competencies
- Indications for operative intervention
- Prevention of corneal blood staining
- IOP control in traumatic glaucoma
Glaucoma Tube Placement
Skills Developed
- Tube shunt placement
- Implant positioning
- Adjunctive device placement (Durysta, Dextenza models)
Clinical Competencies
- Management of traumatic glaucoma
- Understanding implant selection
- Post-traumatic IOP management strategies
Vitrectomy & IOFB Removal / Fish Hook Removal Strategies
Limit 10
Vitrectomy & IOFB Removal
NOTE: This is a highly technical course and most appropriate for those in vitreoretinal fellowship or practicing as a vitreoretinal surgeon.
Skills Developed
- Pars plana vitrectomy setup
- IOFB removal using forceps and magnet
- Use of perfluorocarbon liquids
- Silicone oil injection
- Chandelier lighting techniques
- EyeSi VR trauma simulation
Clinical Competencies
- Posterior segment trauma reconstruction
- Staged vs immediate intervention planning
- Management of complex vitreoretinal trauma
Fish Hook Removal Strategies
Skills Developed
- Fish hook removal from posterior segment & anterior segment
- Pars plana vitrectomy setup
- Use of perfluorocarbon liquids
- Silicone oil injection
Clinical Competencies
- Management of complex fish hook injuries to the globe
- Posterior segment trauma reconstruction
- Staged vs immediate intervention planning
- Management of complex vitreoretinal trauma
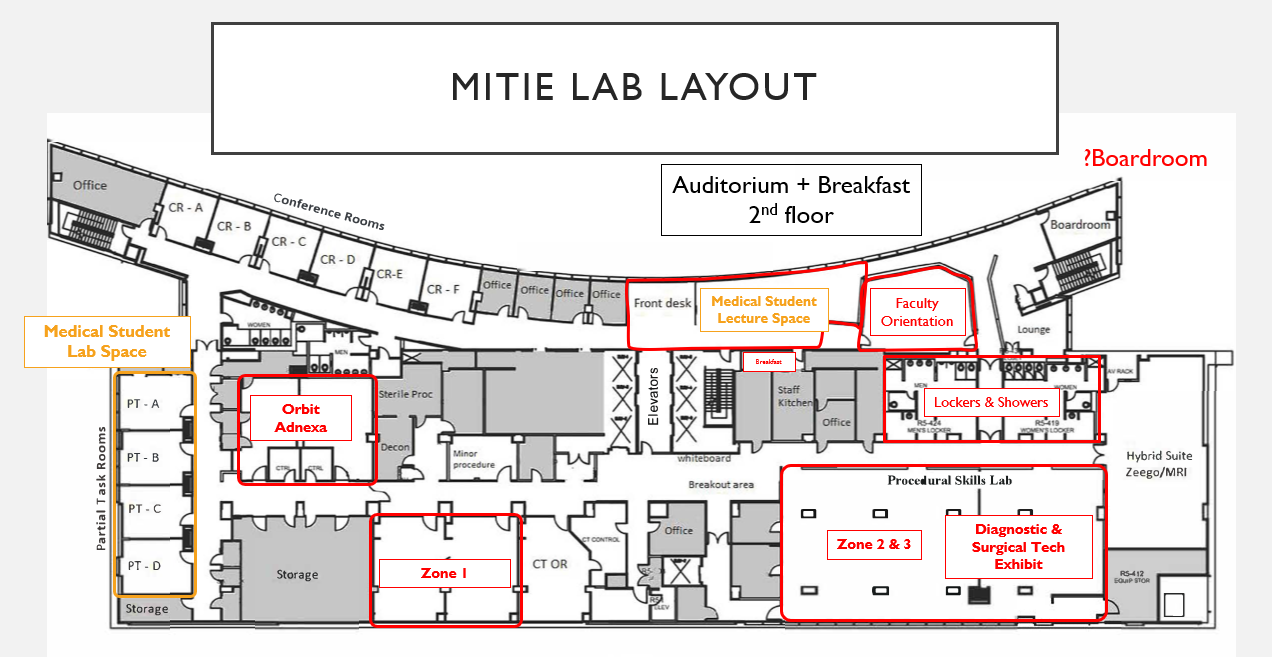
Damage Control Lab Map
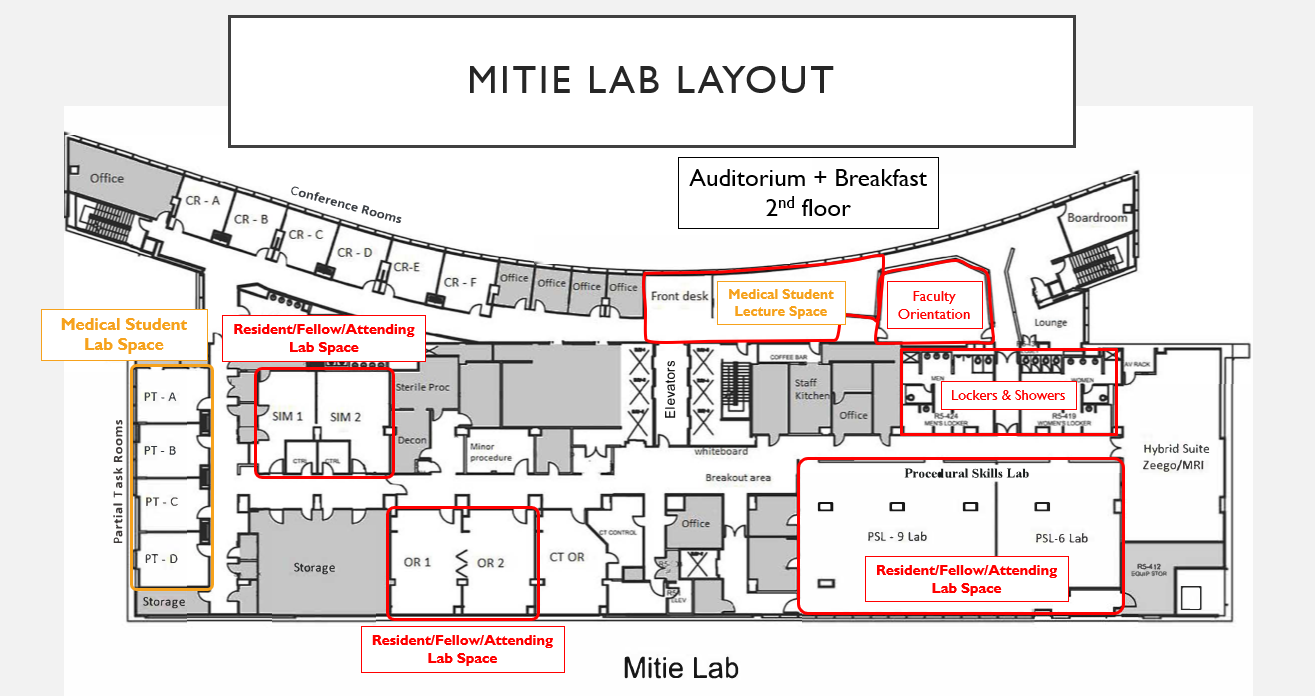
Early Career Lab Map